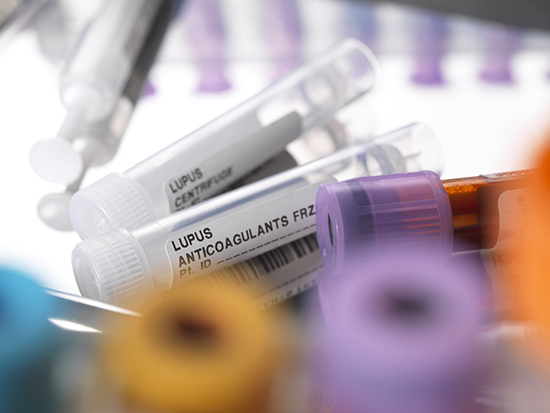
 Lupus, an autoimmune disease that can attack any part of the body, can be confounding because patients often respond differently to the same treatment, and they vary widely in the severity of their symptoms.Nine out of 10 patients with systemic lupus erythematosus — the autoimmune disease also known as SLE — are females. Black women have the highest concentration of disease severity, and they are two to three times more likely to suffer SLE than are white women. The disease usually strikes during childbearing years, ages 15 to 45.
Lupus, an autoimmune disease that can attack any part of the body, can be confounding because patients often respond differently to the same treatment, and they vary widely in the severity of their symptoms.Nine out of 10 patients with systemic lupus erythematosus — the autoimmune disease also known as SLE — are females. Black women have the highest concentration of disease severity, and they are two to three times more likely to suffer SLE than are white women. The disease usually strikes during childbearing years, ages 15 to 45.
To help Black women with SLE, the University of Alabama at Birmingham and two other institutions have received a three-year, $3 million Global Team Science Award from the Lupus Research Alliance. The research will focus on better understanding this difficult disease, where patients often respond differently to the same treatment and vary widely in the severity of their symptoms.
Ignacio Sanz, M.D., chief of Rheumatology at Emory University School of Medicine, leads the multidisciplinary team. His Emory colleagues, together with research teams at UAB and the Medical University of South Carolina, or MUSC, will focus specifically on African American patients, identifying the characteristics of the B cells and plasma cells that create attacking antibodies in the development and progression of severe lupus. The project will define how the different characteristics of these cells correspond to patients’ responses to treatment.
A key to this research by UAB, Emory and MUSC is their access to a unique cohort of Black SLE patients from the American South, using large cohorts composed of rural and urban patients who receive care at the three institutions.
At UAB, this includes the SLE Clinic, which is enriched for severe patients from Alabama’s rural Black Belt and from Birmingham’s urban communities. At Emory, this includes the Georgians Organized Against Lupus cohort, the largest community-based Black SLE cohort in the nation, with urban and rural Black Belt patients who have high poverty and disproportionately poor outcomes. At MUSC, 30 percent of the MUSC SLE Program patients are from the Gullah cohort, a group unique in their low white admixture, their genetic homogeneity and a double familial prevalence of lupus. The Gullah are Blacks who live in the Lowcountry of Atlantic states from Georgia to North Carolina, both on the coastal plain and on the Sea Islands.
SLE results from harmful antibodies made by a patient’s immune system. These can attack any part of the body, including kidneys, brain, heart, lungs, blood, skin and joints. B cells are precursors to plasma cells, the cells that produce the damaging antibodies. The SLE B cell signature is particularly accentuated in Black patients with severe disease, yet major gaps in knowledge to understand the different types of SLE clinical disease still persist.
The researchers say knowledge gained from these studies will greatly enhance understanding of SLE pathogenesis and differences in clinical manifestations, outcomes and therapeutic responses. Moreover, this knowledge will enable clinical investigators to more precisely design and evaluate clinical studies and standard-of-care treatments, with the ultimate goal of safer and more effective personalized treatments.

Fran Lund, Ph.D.UAB investigators for the award, “Linking different B cell types to lupus symptoms, progression and response to therapy,” are Fran Lund, Ph.D., Alex Rosenberg, Ph.D., Winn Chatham, M.D., and Troy Randall, Ph.D., all researchers in the UAB Marnix E. Heersink School of Medicine.
Lund is the Charles H. McCauley Professor of Microbiology and founding director of the UAB Immunology Institute, a cutting-edge and interdisciplinary hub for faculty, researchers, clinicians, health policy experts and educators to advance the study of immunology and improve human health through immune-based therapies. Chatham, a professor of medicine and the Louis W. Heck Clinical Scholar in Rheumatology, is director of the UAB SLE Clinic. Randall, a professor of medicine, holds the Meyer Foundation William J. Koopman, M.D., Endowed Chair in Immunology and Rheumatology. Rosenberg is an associate professor of microbiology.
In addition to Sanz and the UAB investigators, the study includes five other researchers at Emory and two at MUSC.
This Lupus Research Alliance grant is one of two $3 million grants that form the first Global Team Science Awards, totaling $6 million, the largest-ever grant from the alliance.
The other award, “Identifying differences in genetic makeup to stratify children with SLE into specific groups,” went to researchers at Boston Children’s Hospital, Toronto Hospital for Sick Children, Brigham and Women’s Hospital, and the Australian National University.
“The Global Team Science Award embodies the Lupus Research Alliance’s strategic priorities of defining lupus heterogeneity, enabling patient stratification, and fostering collaborative global research and technology teams,” said Teodora Staeva, Ph.D., chief scientific officer at the alliance. “These first two projects, selected from among many compelling proposals, examine important underlying mechanisms of the autoimmune response and point the way to potential new treatment approaches.”