By Tehreem Khan
UAB News
In January 2022, the University of Alabama at Birmingham Marnix E. Heersink School of Medicine announced the first peer-reviewed research outlining the successful transplant of genetically modified pig kidneys into a brain-dead human individual.
Notably, the study recipient, Jim Parsons, had two genetically modified pig kidneys transplanted in his abdomen after his native kidneys were removed. This research was successful because Parsons opted to be an organ donor while he was living, a choice that will forever impact the course of transplantation and saving lives. Although his organs were not viable for transplantation, Parsons’ body was donated to science after his family agreed to allow him to be part of the world’s first-of-its-kind xenotransplantation study with Legacy of Hope at UAB Hospital.
While this research has proved to be groundbreaking in the history of animal-to-human transplantation and will complement traditional human-to-human transplantation, it sheds light on why xenotransplantation exists: to address the organ shortage crisis affecting millions of Americans yearly. A critical way to address the organ shortage crisis is through organ donation.
Organ donation and its uses
An organ donor is someone who has decided to donate their organs and/or tissues upon death to others who may need a new heart, lungs, liver, kidneys, pancreas and/or small bowel to save their life. Many recipients are in need of tissues, such as skin, bones, tendons, ligaments and heart valves. In lifesaving and life-enhancing application, an example of donation could be a person’s skin being provided to treat and improve the quality of life of severe-burn patients, while bone can be used to treat orthopedic injuries and cancer patients.
Most often, organ donation takes place after brain death has been determined or after the family chooses to withdraw life-sustaining therapies.
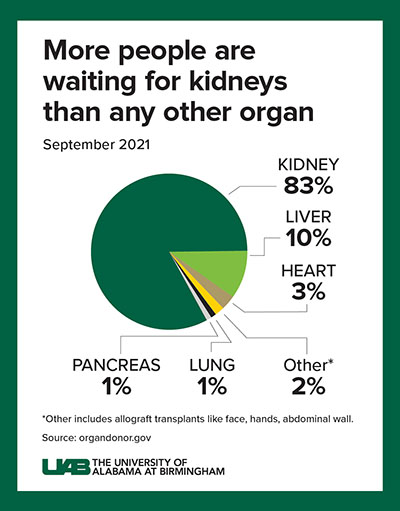
Kidney disease is the leading cause of death in United States adults — even more prevalent than deaths caused by cancers like breast or prostate, according to the National Institute of Diabetes and Digestive and Kidney Diseases.
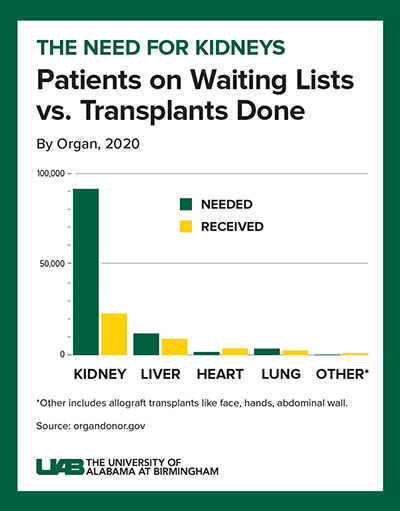
Although transplantation is the gold standard treatment for end-stage kidney disease, fewer than 25,000 kidney transplants are performed each year in the United States, and 240 Americans on dialysis die every day. According to the Organ Procurement and Transplant Network, more than 110,000 individuals are waiting for a lifesaving transplant; of those, nearly 1,300 Alabamians are waiting.
“The generosity of an individual donor can save up to eight lives through organ donation and countless others through tissue donation,” said Legacy of Hope Director of Education Ann Rayburn. “This impact can be seen in the way that many recipients live their lives for years to come, and how a donor’s family can take pride in knowing their loved one made such a difference.”
Many of the deaths of those waiting for organs could be prevented if an unlimited supply of organs were available to meet patient demand. This justifies the demand for an increase in the number of registered organ donors and could save millions of lives.
Becoming an organ donor is a simple process that can save lives. To register or update your organ donation status, visit Legacy of Hope’s registration website or say “yes” in-person at a motor vehicle department.
Conversations about organ donations
Organ donation awareness and education have expanded in recent years. However, as the waiting lists for organ donations continue to grow, it is becoming more vital than ever to have conversations about organ donation with loved ones.
“It may seem daunting to ask a loved one what they would prefer to do with their organs if they pass away, but that conversation doesn’t have to be hard,” Rayburn said.
Rayburn suggests simply telling family and friends about organ donations and the decision to save lives after death by being an organ donor. She notes that the impact of this candid conversation may even encourage others to make plans for becoming an organ donor and/or making sure they are registered.
“Having such conversations gives the family confidence in the donor registry,” Rayburn said. “It also gives the family an opportunity to talk through any questions they may have. By understanding more about why you made this choice, it may be an inspiration to other family members, and they may register to be donors too.”
For some, balancing the dignity of the human body and organ donations is top-of-mind. Legacy of Hope ensures family satisfaction through the availability of visitation and viewing of the body post-donation.
Learn more about the uses of organ donation.
“We are committed to ensuring that families know their loved ones are treated with respect and dignity,” Rayburn said.
Testimonials are an efficient way to encourage residents to help save lives. In Alabama, there are about 1,500 men, women and children waiting for an organ transplant, with each person having a unique story, a family that loves them and a life to live.
“While the waiting list is long, we have to remember that numbers don’t tell the full story. Each number represents a person with a story,” Rayburn said. “When we share stories, people can make a connection and be motivated to register to donate.”
 Getting involved
Getting involved
There are many ways to get involved in this noble cause of saving lives, including registering to be an organ donor, encouraging friends and family to do it, and engaging in conversations educating others about what it means to be a donor.
Many Americans say they want to be organ donors but do not get around to acting on their intentions. Helping these potential donors take action and register could prolong the lives of others significantly. Signing up to be an organ donor has been made easy in Alabama by Legacy of Hope in partnership with UAB Medicine. To register now or update your organ donor status, visit their registration website or simply say “yes” when you visit a motor vehicle department in-person.
UAB Medicine recently surpassed 16,000 total organ transplants in February 2022. During the past half-century, the UAB Comprehensive Transplant Institute has pioneered many advances, including groundbreaking research, new medicines and innovative techniques. Patients from across the country — 44 states — have come to UAB for organ transplantation, making UAB a major national player in the field. UAB has also performed more kidney transplants in African Americans than any other transplant center in the U.S.
The focus of UAB’s xenotransplantation program is to address the organ shortage by safely transplanting genetically modified pig kidneys into humans with kidney failure. Learn more.




