From wire reports
(NAPS) — If you’re like many Americans, you may have heard about the BRCA gene and wondered what it is and whether it is something that could affect you and your family. Here are a few facts.
BRCA is short for “BReast CAncer susceptibility gene.” There are two main types of BRCA gene, BRCA1 and BRCA2. When these changes are present, a woman’s risk of developing breast and ovarian cancers, as well as some other types of cancer, is greatly increased. However, mutations in the BRCA genes are rare, and occur in less than 1 percent of women. A BRCA test is a blood test that looks for mutations, or changes that might be harmful, in these genes.
Who is at risk?
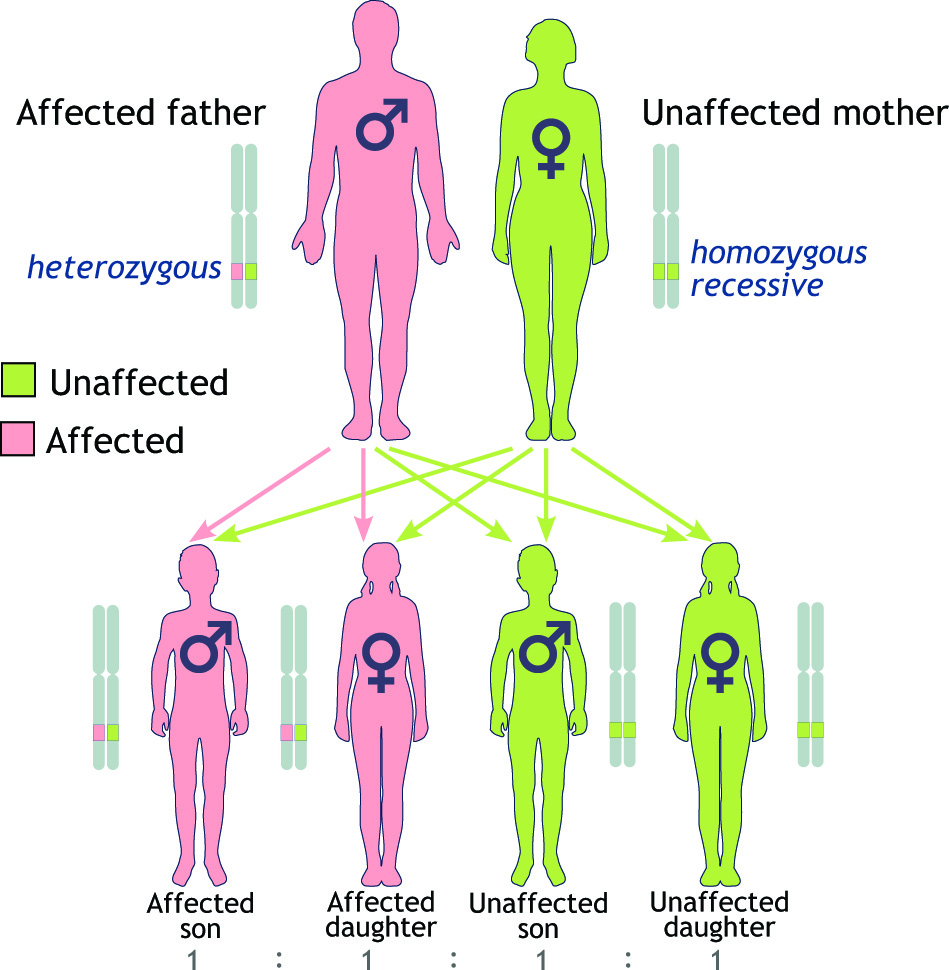
Mutations in the BRCA gene are hereditary, so they run in families. Most women — more than 90 percent — do not have a family history that puts them at increased risk of having a BRCA mutation.
You are at increased risk of having a BRCA mutation if you are of Ashkenazi Jewish descent or if there is a history of certain types of cancer in your family. For example, you are at increased risk if there have been multiple cases of breast cancer in your family, you have a male relative with breast cancer or you have a family member who has had any of the following: a breast cancer diagnosis before age 50, breast cancer in both breasts or two types of BRCA-related cancer — such as both breast and ovarian cancer.
According to the U.S. Preventive Services Task Force, a woman with a family history of BRCA-related cancer should be screened by her primary care doctor or nurse to determine if she is at increased risk of having a BRCA mutation. During this screening, the doctor or nurse will ask questions about the history of BRCA-related cancer in a woman’s family. After screening, women who are found to be at increased risk should see a genetic counselor, a type of health care professional who specializes in genes and disease. A genetic counselor may recommend BRCA testing based on that counseling. Before this type of screening, most doctors will first test a family member with known breast or ovarian cancer for a BRCA mutation, if possible.
The BRCA test is not a test for cancer itself, but rather a test for the gene mutation and a positive test does not mean that a woman will definitely get cancer. For women who are at increased risk of having a BRCA mutation, genetic counseling and genetic testing can help them determine their best course of action based on their risk.
The BRCA test is only recommended for women who are at increased risk for certain types of cancers. This is because the test does not always provide a clear answer — results are often inconclusive, which can lead to increased anxiety.
All women can reduce
their cancer risk
While a BRCA gene mutation can be frightening, it is not something that most women need to worry about. All women can reduce their risk of cancer by adopting healthy lifestyle habits, such as limiting alcohol, not smoking, being physically active and maintaining a healthy weight. Receiving regular mammograms is also an important tool to help identify breast cancer early. The U.S. Preventive Services Task Force recommends mammograms every other year for women aged 50 to 74 and for some women in their 40s based on their values about the benefits and harms of screening.
Recommendations
to protect your health
The U.S. Preventive Services Task Force is an independent group of national experts in primary care, prevention, and evidence-based medicine. The aim of the Task Force’s work is to evaluate and identify critical preventive health services that a primary care professional can perform.
For more information on the Task Force and to read its full report on risk assessment, genetic counseling and genetic testing for BRCA-related cancer in women, visit www.uspreventiveservicestaskforce.org.
If you have a history of breast or ovarian cancer in your family, talk to your doctor about genetic screening.