By Bob Shepard
UAB News

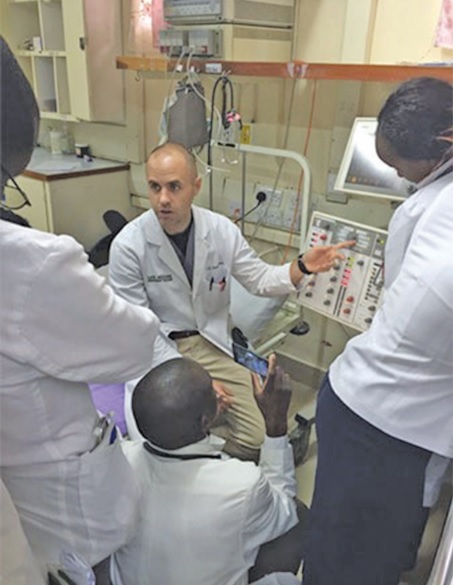
UAB’s Scott Irvine, M.D., director of the International Emergency Medicine Fellowship, works on simulation training with Kenyan residents and interns.
For five days this fall in Kenya, emergency doctor Scott Irvine was a full-time teacher. Irvine, director of the International Emergency Medicine Fellowship in the University of Alabama at Birmingham Department of Emergency Medicine, spends a lot of time teaching while in the States, working with medical students and residents during duty shifts in the UAB emergency department. This was different.
“This event, the Kenya Emergency Medicine and Critical Care Conference, was the first large-scale teaching symposium the International Emergency Medicine Fellowship conducted overseas,” Irvine said. “We enrolled 42 attendees for the weeklong conference — mostly Kenyan surgical residents and general medicine interns — conducting classes on critical care and trauma.”
Kenya’s medical system is relatively advanced, but the East African nation does not have a training program in emergency medicine for its young physicians, a common situation in sub-Saharan Africa. That provided an environment tailor-made for the UAB fellowship.
The fellowship was created in 2012 to equip emergency physicians to deliver medical care in the underdeveloped and developing world. This includes specialty training in infectious disease and tropical medicine, humanitarian aid, and austere medicine. Graduates are also expected to gain competency in coordinating with government and nongovernment initiatives, and to work closely with local practitioners.
Irvine was the first to complete the one-year course of study and now heads the program, which has graduated five fellows. It features a variety of independent study, research and course work, including the Gorgas Diploma Course, a comprehensive nine-week tropical medicine course in Peru run by the UAB School of Medicine. Fellows spend an additional six to eight weeks in the field, seeing patients and teaching local medical providers at the bedside.
Irvine teaches advanced critical care techniques to residents and interns at Tenwek Hospital in Kenya.
“We wanted to branch out from training our own fellows to offering advanced education classes in countries around the world,” Irvine said. “We are expanding our educational footprint and hope to have a long-term impact on medical care in Kenya, particularly in emergency medicine, as a result of the conference.”
The 10-member team of instructors in Kenya included physicians from Canada and Kenya, a graduated fellow now in Kentucky, and Chris Greene, M.D., a UAB assistant professor in emergency medicine and the third fellow to finish the program.
“Kenya has competent and capable physicians and residents who are practicing a high level of critical care medicine with limited resources,” Greene said. “Lack of resources and lack of advanced training does limit what they can do in areas like advanced cardiac management or sepsis care. We were privileged to be able to present new knowledge about concepts such as advanced ultrasound, stroke care and neurocritical care.”
Home base for the conference was Tenwek Mission Hospital in Bomet, Kenya, a major regional teaching hospital with 350 beds. Irvine says Kenyan authorities were excited to have external partners to help prepare their young physicians in critical care.
“We received a great evaluation from our students, suggesting that they hoped to have similar educational opportunities on a regular basis,” Irvine said. “We did simulation training to test their practical knowledge, which went very well. We were impressed by how much they absorbed over the week and how that translated to the bedside.”
Irvine says the next steps are to follow various markers to see if the training has had an impact on mortality rates, for instance, or if there is a decrease in patient-ventilator days. The program will continue to do assessments at six months and one year to see if the knowledge gained by the training has been sustained. Irvine also hopes the conference will be an annual undertaking.
“Our goal would be to expand to other hospitals in other nations eventually, by using these experiences to build a model that is replicable in other settings,” Irvine said.
The team noted that Kenya is beginning to experience an increase in noncommunicable diseases common in the developed world, such as Type 2 diabetes, heart disease, obesity and high blood pressure — diseases for which Western physicians have a great deal of experience.
“I really enjoyed working with clinicians from different cultures who have different expertise due to their patient populations,” Greene said. “It is gratifying to work with them on the things they need to know while at the same time learning from them. We are working together to bring medicine to where it is most effective and most life-changing.”